 |
 |
 |
| Fig. 01 | Fig. 02 | Fig. 03 |
There two principles in the moist wound healing, no disinfectants over the wound and keeping the wound in moist environment. Lacerations, abrasions, crush injuries and burn are all treated with this moist wound treatment method and the wounds heal faster with less scarring.
Disinfectants such as povidone iodine, sodium hypochlorite, and hydrogen peroxide should never be used over wound surface, as they are toxic to cells.
The idea of moist healing was born in 1962 when George D. Winter discovered that epithelialization would proceed twice as fast in a moist environment than under a scab.
Cell growth needs moisture and the principle aim of moist wound therapy is to create and maintain optimal moist conditions. Cells can grow, divide and migrate at an increased rate to optimize the formation of new tissue. During this phase of wound healing an aqueous medium with several nutrients and vitamins is essential for cell metabolism and growth.
The wound exudate serves as a transport medium for a variety of bioactive molecules such as enzymes, growth factors and hormones. The different cells in the wound area communicate with each other via these mediators, making sure that the healing processes proceed in a coordinated manner.
Wound exudate also provides the different cells of the immune system with ideal conditions to destroy invading pathogens such as bacteria, foreign bodies and necrotic tissues, diminishing the rate of infection.
Moist wound treatment is known to prevent formation of a scab, allowing epithelial cells to spread horizontally outwards through the thin layer of wound exudate to rapidly close the wound. In addition, pain is significantly reduced when wounds are covered with an occlusive dressing. Concerns that moisture in wounds would increase the risk of clinical infection over traditional therapies are unfounded. The use of hydrocolloid occlusive dressings in maintaining a moist wound environment has proved to be a useful adjunct in facilitating wound healing.
Actual components of wound care include cleaning, dressing, determining frequency of dressing changes, and reevaluation. Dead tissue and debris can impede healing; therefore the goal of cleaning the wound is the removal of dead tissue and debris..
In summary, advantages of moist wound treatment over dry wound treatment are as follows:
At first the wound have to be cleaned with tap water. Then the wound is covered with an alginate dressing and covered with an adhesive tape, which can be non-sterile. The next day, the wound is evaluated. After the removal of the dressing, it is washed with tap water. The next steps vary by locations; the facial wound is covered with a hydrocolloid dressing and other wounds need to be covered with multi-layered dressings (i.e. , Plusmoist(TM) ). After the dressings change, the patient removes and changes the dressings everyday. The goal of the treatment is an exudate-free and fully covered epithelialization. Exposure of the wound to sunlight should be avoided, because ultraviolet light enhances pigmentations of the wound scar.
A contaminated wound have to be cleaned after local anesthesia is applied. The foreign body must be removed completely. After that, the procedure described as above is performed.
Deep wounds with exposure of fat, muscles or bones, are also treated in the same manner.
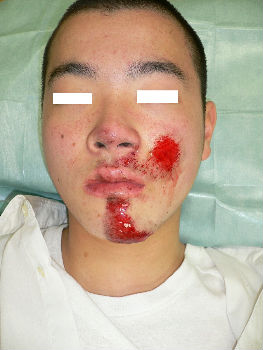
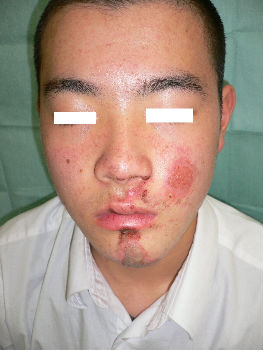
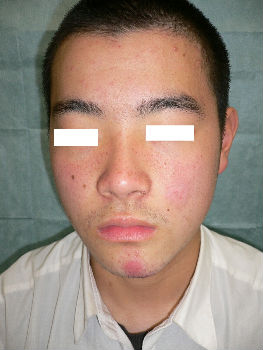
A facial abrasion wound
A 16-year-old man fell while riding his bicycle and he presented to our hospital. At the examination, he had abrasion with bleeding on his left cheek and chin (Fig. 01). Figure 1B shows the state of the injury the next day. With hydrocolloid dressings for three days, epithelialization is completed (Fig. 02). Ten days following the injury, the wound is healed without scarring (Fig. 03).
 |
 |
 |
| Fig. 01 | Fig. 02 | Fig. 03 |
In the past, lacerations were treated with suturing. But, we have found that most lacerations, especially those on the face of child, could be treated without suturing.
A bleeding wound is managed with pressure hemostasis at first. After hemostasis, the wound edges are aligned and fixed with tape. We use Leukostrip(TM) and Steristrip(TM) for closure, and keep firm pressure over the wound with bandage to prevent hematoma. On the next day, all dressings are removed, and the condition of the wound is examined. After no sign of infection is confirmed, the wound is taped again.
For finger or hand injury, we recommend using alginate dressing with film plasters. On day two and following, the wound is covered with Plusmoist(TM). On average, lacerations are healed in 7 to 10 days with this method.
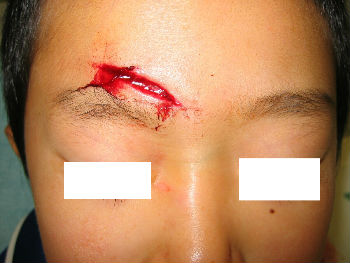
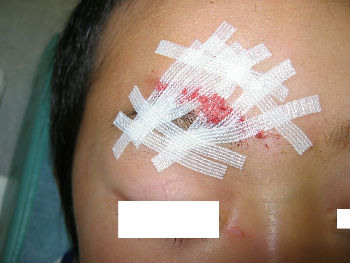
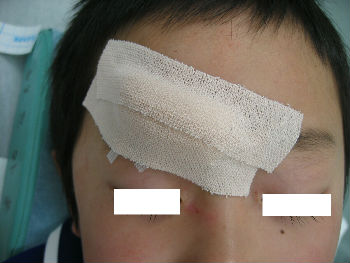
A 4-year-old boy fell down and hit his forehead against the edge of a piece of furniture. The right forehead laceration reached the layer of the periosteum (Fig.04). We closed the wound with plaster to stop the bleeding by pressing (Fig.05). applying the layer of the rolled gauze shed further pressure (Fig.06). The following day, Steristrips with compression were applied. This picture (Fig.07) shows the status of the wound on day 3, the wound is closed without hematoma. We gave instructions to family members about further management of the wound at home.
 |
 |
 |
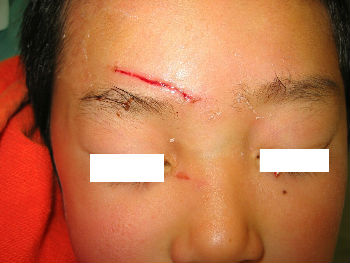 |
| Fig. 04 | Fig. 05 | Fig. 06 | Fig. 07 |
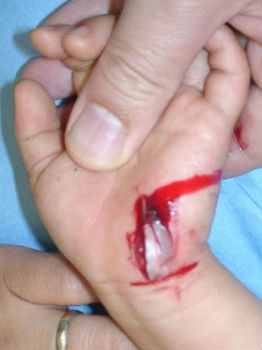
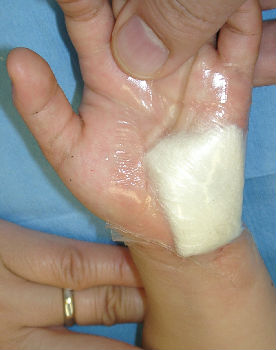
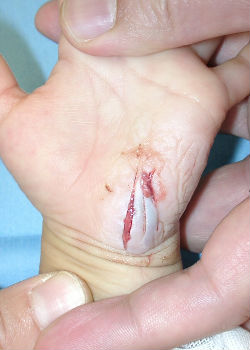
2-year-old girl cut her hand playing with umbrella parts. She was immediately taken to our hospital. Lacerations on her left hypothenar area (Fig.08) was treated with an application of Alginate dressings (Fig.09). From day2 to day7, we treated the wound with hydrocolloid dressings (Fig. 10). Fig. 11 shows well healed wound on day15.
 |
 |
 |
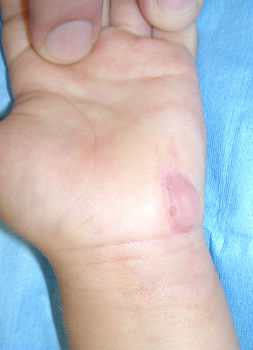 |
| Fig. 08 | Fig. 09 | Fig. 10 | Fig. 11 |
With moist wound treatment, even third-degree burns can be treated without skin-graft, and when the burn is covered completely(preventing exposure to open air) pain is not experienced. Patients with third-degree burns can remain active and can be managed as outpatients. They do not need intravenous infusion or hospitalization.
On the initial visit, blister membranes have to be removed, because they may be infected. After removal of the membrane, we cover the burn with plastic wrap coated with petroleum jelly. Next we apply gauze over the plastic wrap and affix with bandages. With the moist dressing, pain is reduced or completely resole within several minutes. Pain killers are usually not prescribed. On the second day, dressings are exchanged with Plusmoist(TM). From day2 and following, dressings are changed once a day. The mild burn wound will heal within several days. Deep third-degree burns heal within months with this moist treatment method.
We encourage patients to move joints and muscles around the wound, because resting causes joint and skin contractures, thus resting should be avoided.
If patients develop fever and pain at the burn site, we prescribe antibiotics not analgesics because the fever and pain indicate wound infection.
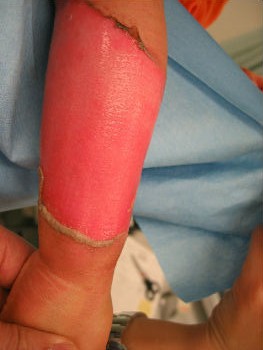
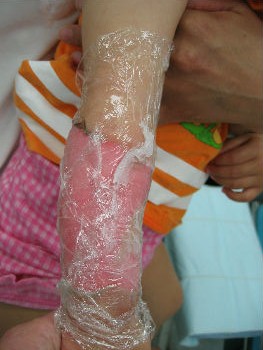
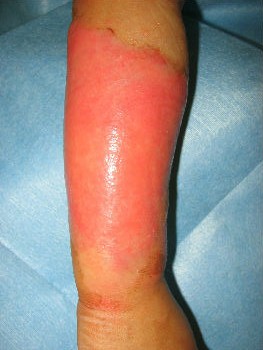
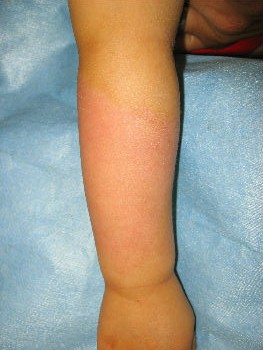
A one-year-old girl tipped a pan filled with hot miso-soup and sustained a burn on her left forearm. She saw a plastic surgeon at a university hospital immediately. The plastic surgeon covered her burn with gauze directly. He told her parents that she needed hospitalization for skin graft, and that without surgery sepsis will develop. Her parents were not satisfied with the recommended treatment plan and searched the internet for better treatment option. They found information about moist environment treatment. They brought her to our wound treatment center. . After removal of the gauze, we noted superficial second-degree burn (Fig. 12). Promptly we covered it with plastic wrap. Upon sealing with the wrap she stopped crying within 10 seconds (Fig.13). Thereafter, we treated her burn with Plusmoist(TM). On day 4 post-burn, there was little exudate (Fig. 14). On day 16, the burn was completely healed without a scar (Fig.15). There was no functional sequela in her arm.
 |
 |
 |
 |
| Fig. 12 | Fig. 13 | Fig. 14 | Fig. 15 |
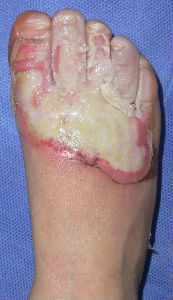
A-two-years-old boy was burned his right foot by hot water. His parents brought him to a plastic surgery of a nearby general hospital. He was treated with silver-sulfadiazine cream and gauze dressing.
Two weeks after the injury, his doctor informed the parents as "Skin graft is indispensable for healing. Gait problem is unavoidable without early skin graft. Sepsis is inevitable without surgery." However, the parents could not agree to the opinion. Afterward the parents got information about moist wound healing via the internet and brought him to our hospital.
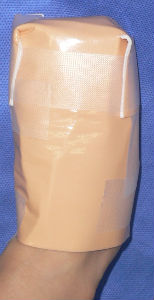
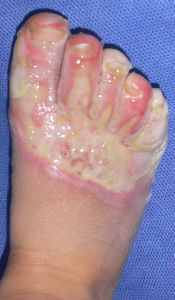
Plusmoist(TM) was just applied without any debridement.
 |
 |
 |
 |
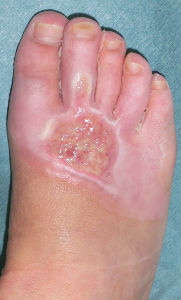
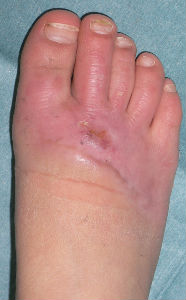
| primary condition coverd with necrotic tissue |
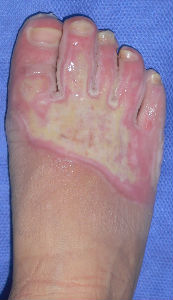
covered with Plusmoist(TM) | 4 days after | 8 days after |
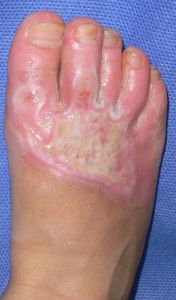 |
 |
 |
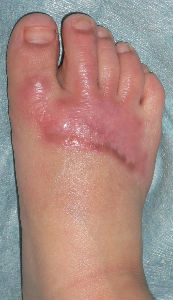 |
| 15 days after | 26 days after | 46 days after | 63 days after with no cicatrical contracture |
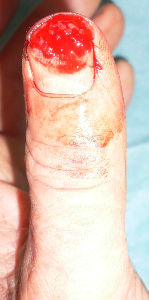
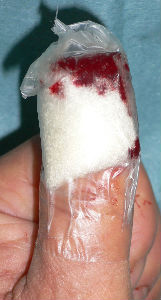
The patient is a 60 years old male worker; suffering from the cut wound of dorsal side of the left thumb visited our hospita. The wound was diagnosed as the defect of the nail plate and nail bed, complicated with the open bone fracture of the distal phalanx.
I attached the sodium alginate dressing. At the initial diagnosis, I removed the blood coagulation, attached the sodium alginate dressing on the wound and enclosed the wound by the film.
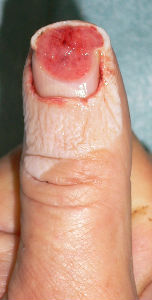
The day after the first visit, his nail bed was embedded by the surrounding healing granulation. I altered the dressing from sodium alginate dressing to Plusmoist(TM).
 |
 |
 |
 |
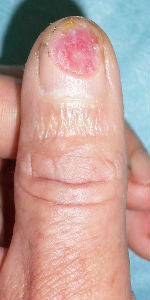 |
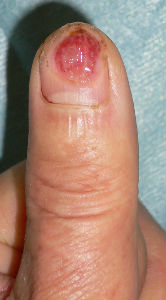
| the first condition | covered with alginate dressing | one day after | 11 days after | 21 days after |
He chanced to re-visit our hospital on 94 days after, and I confirmed the complete reconstitution of the left thumb nail. The nail plate of his left thumb fully covered the nail bed, and fully recovered the intact nail form.
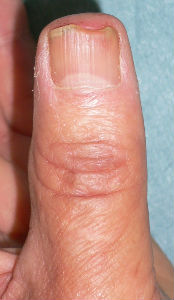 |
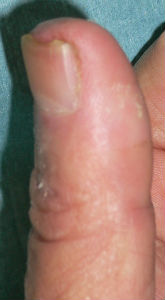 |
| 94 days after | lateral view |
#1. Miliaria (an itchy rash of small raised red spots) or impetigo(a superficial skin infection)
Skin is one of the excretory organs. Sealing the skin causes dysfunction of excretion. It can cause miliaria or impetigo. For preventing these skin problems, dressings have to be changed everyday after washing the wound with plenty of tap water.
#2. Wound infection
Detection of infection is important. Infection does not mean that bacteria are found in the wound. Signs of infection include pain and/or redness at the site. If the wound becomes infected, the infected site must be removed. Antibiotics are not needed for the patient whose symptoms disappear following these measures.
#3. Granuloma(thickening of skin at the wound site) formation
Sealing the wound with steroid ointment covered dressing, the granuloma becomes flat and the wound resumes epithelialization(healing of the wound) .
Makoto Natsui (MD), e-mail, JAPAN