

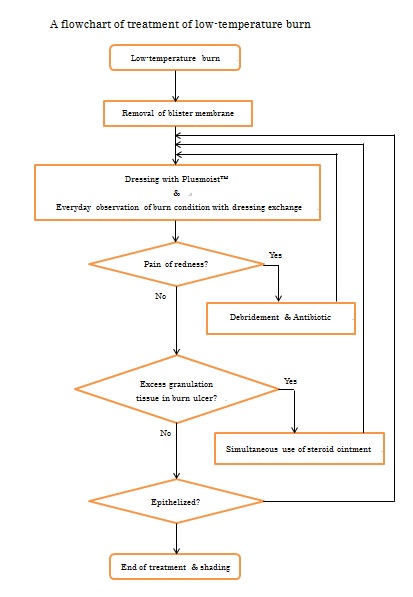
There were two principles in the moist wound healing, no disinfectants over the wound and keeping the wound in moist environment. Lacerations, abrasions, crush injuries and burn are all treated with this moist wound treatment method and the wounds heal faster with less scarring.
Disinfectants such as povidone iodine, sodium hypochlorite, and hydrogen peroxide should never be used over wound surface, as they are toxic to cells.
The idea of moist healing was born in 1962 when George D. Winter discovered that epithelialization would proceed twice as fast in a moist environment than under a scab.
Cell growth needs moisture and the principle aim of moist wound therapy is to create and maintain optimal moist conditions. Cells can grow, divide and migrate at an increased rate to optimize the formation of new tissue. During this phase of wound healing an aqueous medium with several nutrients and vitamins is essential for cell metabolism and growth.
The wound exudate serves as a transport medium for a variety of bioactive molecules such as enzymes, growth factors and hormones. The different cells in the wound area communicate with each other via these mediators, making sure that the healing processes proceed in a coordinated manner.
Wound exudate also provides the different cells of the immune system with ideal conditions to destroy invading pathogens such as bacteria, foreign bodies and necrotic tissues, diminishing the rate of infection.
Moist wound treatment is known to prevent formation of a scab, allowing epithelial cells to spread horizontally outwards through the thin layer of wound exudate to rapidly close the wound. In addition, pain is significantly reduced when wounds are covered with an occlusive dressing. Concerns that moisture in wounds would increase the risk of clinical infection over traditional therapies are unfounded. The use of hydrocolloid occlusive dressings in maintaining a moist wound environment has proved to be a useful adjunct in facilitating wound healing.
Actual components of wound care include cleaning, dressing, determining frequency of dressing changes, and reevaluation. Dead tissue and debris can impede healing; therefore the goal of cleaning the wound is the removal of dead tissue and debris..
In summary, advantages of moist wound treatment over dry wound treatment are as follows:
At first the wound have to be cleaned with tap water. Then the wound is covered with an alginate dressing and covered with an adhesive tape, which can be non-sterile. The next day, the wound is evaluated. After the removal of the dressing, it is washed with tap water. The next steps vary by locations; the facial wound is covered with a hydrocolloid dressing and other wounds need to be covered with multi-layered dressings (i.e. , Plusmoist(TM) ). After the dressings change, the patient removes and changes the dressings everyday. The goal of the treatment is an exudate-free and fully covered epithelialization. Exposure of the wound to sunlight should be avoided, because ultraviolet light enhances pigmentations of the wound scar.
A contaminated wound have to be cleaned after local anesthesia is applied. The foreign body must be removed completely. After that, the procedure described as above is performed.
Deep wounds with exposure of fat, muscles or bones, are also treated in the same manner.
A facial abrasion wound
A 16-year-old man fell while riding his bicycle and he presented to our hospital. At the examination, he had abrasion with bleeding on his left cheek and chin. With hydrocolloid dressings for three days, epithelialization is completed. Ten days following the injury, the wound is healed without scarring.
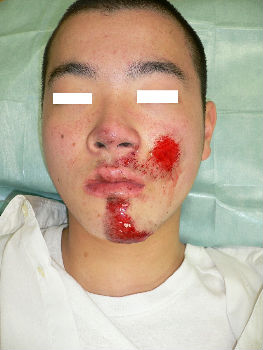 |
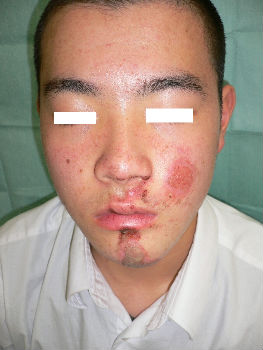 |
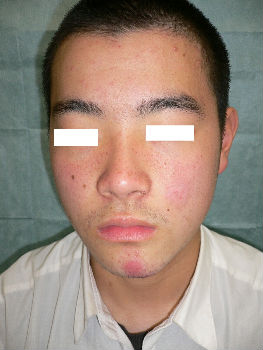 |
| primary condition | 3 days after | 10 days after |
A 70-year-old woman presented with dog bite avulsion to her upper lip. She lost about seventy percent of upper red lip and a part of white lip including the vermilion border. Through the wound, we could see the cut edges of the obricularis oris muscle in both sides. In the center of the wound, there was a part of mucosa left and she lost most of the obricularis oris muscle.
She said that blood spouted from the wound directly after injury. We supposed that the both side of labial arteries were cut off in the muscle stumps. When she arrived the hospital, hemostasis had been achieved.
We gave her the infusions of antibiotic Cefazolin only one day. Day 2, we confirmed that no signs of infection were seen. We did not use antibiotics during following days.
We used Gentamicin ointment for topical use, and sealed the wound with the dressing which had brand name Tielle(tm) over the applied ointment.
Day 4, the wound was covered with proper granulation. Days 7, we changed the dressing materials to Allevyn(tm) and ointment.
Day 11, the defect of mucosa and skin reduced rapidly. Her lip was regenerated to form normally. We changed dressing materials to Duoactive ET(TM) only.
Day 21, the wound closed completely and her lip formed normally. With regenerated lip, she could close her mouth, eat without problems and speak fully functionally.
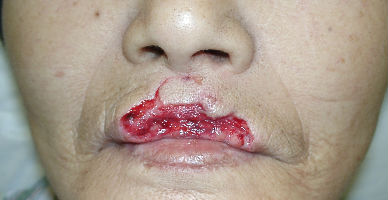 |
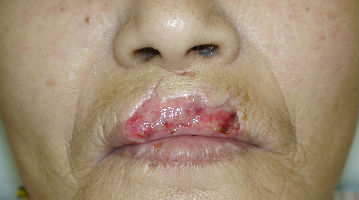 |
| primary condition | 4 days after |
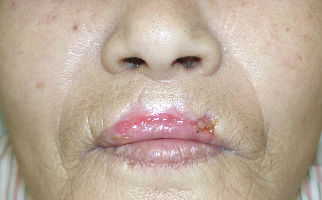 |
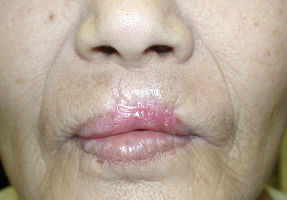 |
| 11 days after | 21 days after |
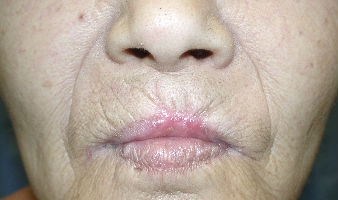 |
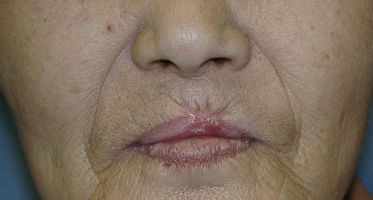 |
| 46 days after | 67 days after |
In the past, lacerations were treated with suturing. But, we have found that most lacerations, especially those on the face of child, could be treated without suturing.
A bleeding wound is managed with pressure hemostasis at first. After hemostasis, the wound edges are aligned and fixed with tape. We use Leukostrip(TM) and Steristrip(TM) for closure, and keep firm pressure over the wound with bandage to prevent hematoma. On the next day, all dressings are removed, and the condition of the wound is examined. After no sign of infection is confirmed, the wound is taped again.
For finger or hand injury, we recommend using alginate dressing with film plasters. On day two and following, the wound is covered with Plusmoist(TM). On average, lacerations are healed in 7 to 10 days with this method.
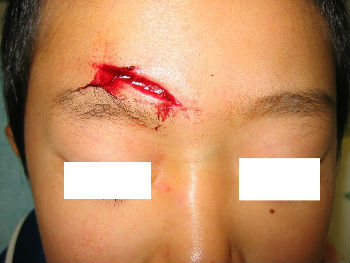
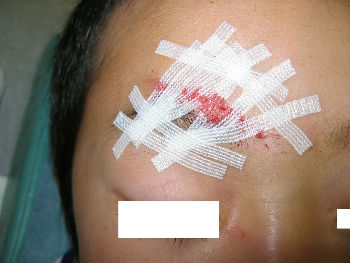
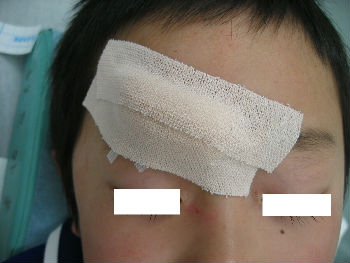
A 4-year-old boy fell down and hit his forehead against the edge of a piece of furniture. The right forehead laceration reached the layer of the periosteum. We closed the wound with plaster to stop the bleeding by pressing. applying the layer of the rolled gauze shed further pressure . The following day, Steristrips with compression were applied. Days 3, the wound is closed without hematoma. We gave instructions to family members about further management of the wound at home.
 |
 |
 |
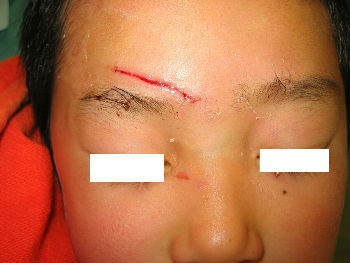 |
| primary condition | wound closure | pressure bandage | 3 days after |
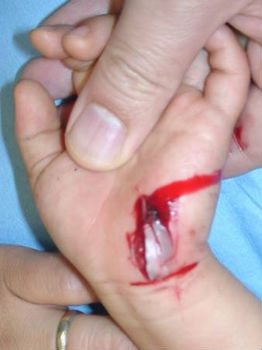
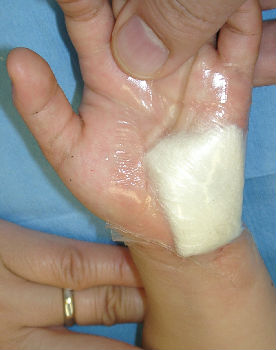
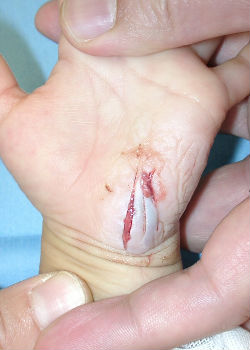
2-year-old girl cut her hand playing with umbrella parts. She was immediately taken to our hospital. Lacerations on her left hypothenar area was treated with an application of Alginate dressings. From day2 to day7, we treated the wound with hydrocolloid dressings. Days 15, wound was well healed.
 |
 |
 |
 |
| primary condition | covered with Alginate dressing | 2 days after | 15 days after |
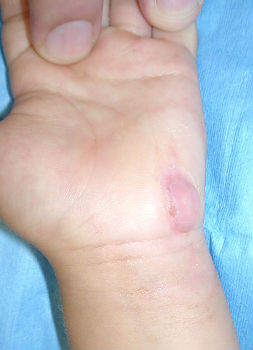
With moist wound treatment, even third-degree burns can be treated without skin-graft, and when the burn is covered completely(preventing exposure to open air) pain is not experienced. Patients with third-degree burns can remain active and can be managed as outpatients. They do not need intravenous infusion or hospitalization.
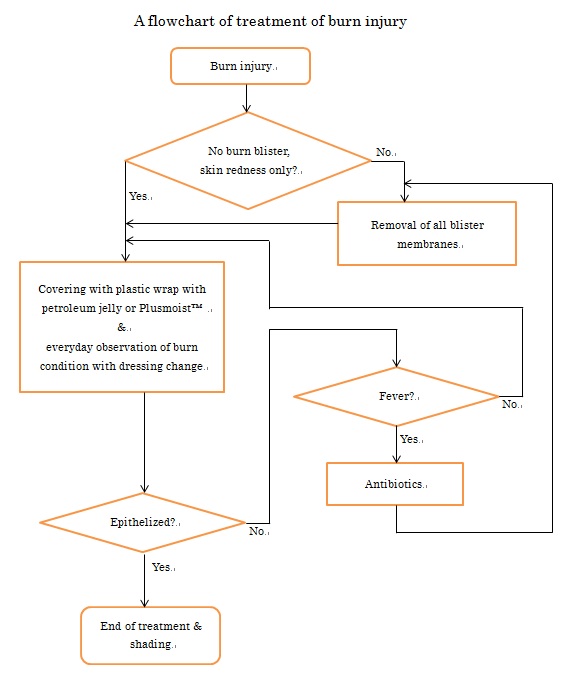
On the initial visit, blister membranes have to be removed, because they may be infected. After removal of the membrane, we cover the burn with plastic wrap coated with petroleum jelly. Next we apply gauze over the plastic wrap and affix with bandages. With the moist dressing, pain is reduced or completely resole within several minutes. Pain killers are usually not prescribed. On the second day, dressings are exchanged with Plusmoist(TM). From day2 and following, dressings are changed once a day. The mild burn wound will heal within several days. Deep third-degree burns heal within months with this moist treatment method.
We encourage patients to move joints and muscles around the wound, because resting causes joint and skin contractures, thus resting should be avoided.
If patients develop fever and pain at the burn site, we prescribe antibiotics not analgesics because the fever and pain indicate wound infection.
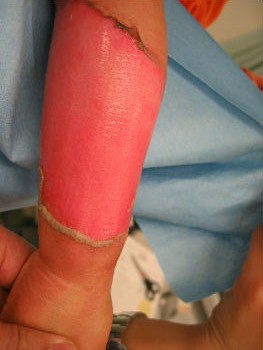
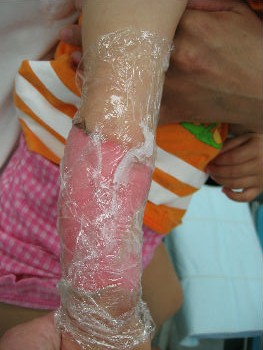
A one-year-old girl tipped a pan filled with hot miso-soup and sustained a burn on her left forearm. She saw a plastic surgeon at a university hospital immediately. The plastic surgeon covered her burn with gauze directly. He told her parents that she needed hospitalization for skin graft, and that without surgery sepsis will develop. Her parents were not satisfied with the recommended treatment plan and searched the internet for better treatment option. They found information about moist environment treatment. They brought her to our wound treatment center. . After removal of the gauze, we noted superficial second-degree burn. Promptly we covered it with plastic wrap. Upon sealing with the wrap she stopped crying within 10 seconds. Thereafter, we treated her burn with Plusmoist(TM). On day 4 post-burn, there was little exudate. On day 16, the burn was completely healed without a scar. There was no functional sequela in her arm.
 |
 |
 |
 |
| primary condition | covered with wrap | 4 days after | 16 days after |
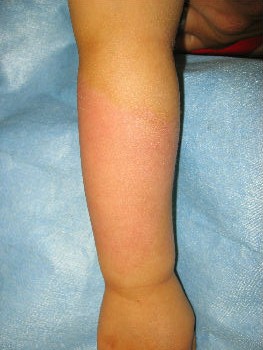
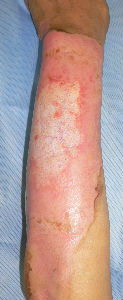
Case: A male patient in his fifties sustained a burn injury on the left forearm and left neck in an accident at work and was treated at a nearby hospital after the initial consultation. However, he was anxious about the treatment at the hospital and visited our department as an outpatient 3 days after the first visit. Pyrexia (38.9°C) was observed at the first visit.
Burn injury was observed circumferentially along the entire left forearm, and a large blister with cloudy fluid covered the lesion. He complained of severe wound pain.
The wound surface was covered with Plusmoist(TM) and white petrolatum applied lightly. In addition, an intravenous drip infusion of Cefamezin (cefazolin sodium hydrate, 2 g) was administered. After completion of the intravenous drip infusion, his body temperature decreased to 37.5°C, and the wound pain disappeared. Therefore, the patient was allowed to go home.
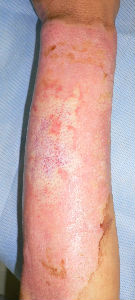
Around day 8, he presented with pyrexia of 37.8°C and mild wound pain, for which intravenous drip infusion of Cefamezin was administered. Pyrexia and wound pain improved after 1-time intravenous drip infusion.
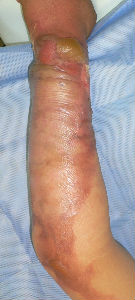
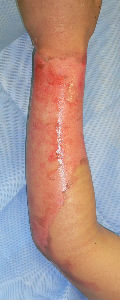
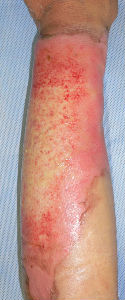
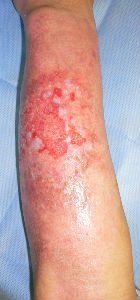
Almost the entire surface on the volarl and dorsal sides showed epithelization; however, epithelization on the ulnar forearm was delayed. On day 30, the burn was considered as third degree, but Plusmoist(TM) was continuously applied.
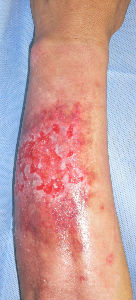
On day 48, insular epithelization was observed even on the lesion that was considered a third-degree burn. All lesions had healed on day 55, and no contracted scar was observed.
 |
 |
 |
 |
 |
| primary condition: dorsal side of forearm |
after removval of blister |
6 days later | 11 days later | 15 days later |
 |
 |
 |
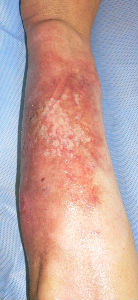 |
| 28 days later | 33 days later | 48 days later: small white spots are epithelization from hair folicles of dermis |
55 days later: no cicatrical contracture |
The skin ulcer on the ulnar surface examined on day 30 might have been diagnosed as a third-degree burn by some physicians who would have considered skin grafting. However, when the image of the same lesion was examined on day 48, it was observed that the wound was not a third-degree burn. This was because the white spots that had developed in the center of the wound were regenerated skin with dermal appendages, including deep follicles resurrected from the lesion. Thus, the wound was not a third-degree burn, but a second-degree burn.
Burns of such depth take usually 40 to 50 days after the injury to regenerate epidermis from the dermal appendage, because it takes a long time for the dermal appendage to regenerate from the damage caused by the initial heat. Thus, until 40 days after injury, it is unknown whether the wound is a third-degree burn or not, and an accurate diagnosis cannot be made.
Accordingly, except in cases in which the skin shows a parchment-like appearance within a few days after the first visit, the diagnosis of a third-degree burn has to be made 40 to 50 days after the injury. In addition, the necessity of a skin graft has to be evaluated after that period. However, when we examine the condition of this patient on day 30, we should conclude that the diagnosis of "this wound is a third-degree burn that cannot be cured exclusively by skin grafting" would be wrong, and thus, skin grafting would be an unnecessary treatment.
In addition, this case also tells us that "the source of infection of the burn wound is the remaining blister fluid (blister membrane)." Blister fluid is usually sterile but becomes a nutritious bacterial medium and a source of infection when even a part of the membrane is broken. Therefore, the blister membrane or the future source of infection has to be removed as much as possible at the first visit in order to prevent an infection.
Moreover, antibiotic administration to prevent an infection is meaningless if the partly broken blister membrane remains in the wound. Of course, the symptoms of cellulitis would temporarily subside, but cellulitis would eventually exacerbate if infected blister fluid of large amounts of bacterial medium remain in the wound.
Furthermore, Plus Moist with white petrolatum (lightly applied) was administered at the first visit, but white petrolatum was only required for the first treatment and not thereafter. White petrolatum was applied for the first treatment in an attempt to halt contact with air as much as possible, and it was not required after the second treatment because effusions adequately covered the wound surface.
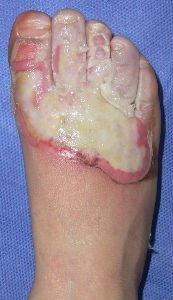
A-two-years-old boy was burned his right foot by hot water. His parents brought him to a plastic surgery of a nearby general hospital. He was treated with silver-sulfadiazine cream and gauze dressing.
Two weeks after the injury, his doctor informed the parents as "Skin graft is indispensable for healing. Gait problem is unavoidable without early skin graft. Sepsis is inevitable without surgery." However, the parents could not agree to the opinion. Afterward the parents got information about moist wound healing via the internet and brought him to our hospital.
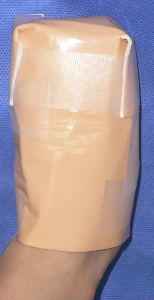
Plusmoist(TM) was just applied without any debridement.
 |
 |
 |
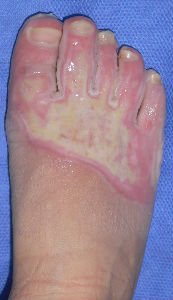 |
| primary condition coverd with necrotic tissue |
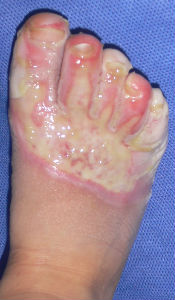
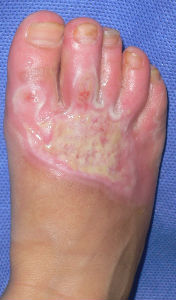
covered with Plusmoist(TM) | 4 days after | 8 days after |
 |
 |
 |
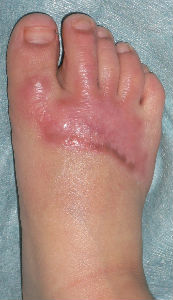 |
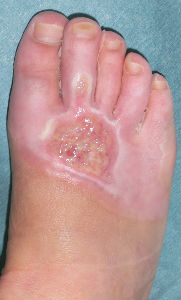
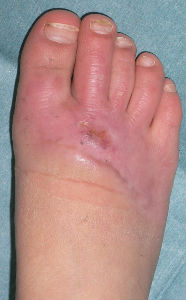
| 15 days after | 26 days after | 46 days after | 63 days after with no cicatrical contracture |
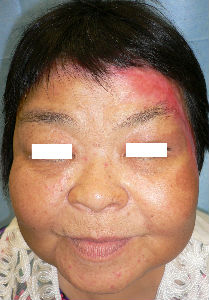
A 60 year-old-woman sustained burns of her face and neck at her home. The stove in the kitchen had ignited her scarf. She was on dialysis. She was diabetic and had self-injection of insulin. The burn day, she went the dialysis center and received primary burn care.
She was suffered from severe diabetes and diabetic renal insufficiency, and was treated hemodialysis at the dialysis center for 5 years.
Day 3, she admitted to the dialysis devision of our hospital and we were consulted about the burn wounds.
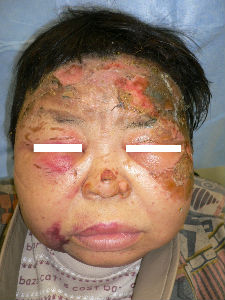
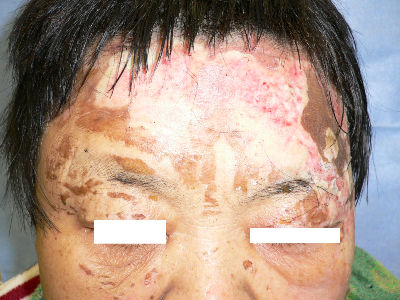
At our first evaluation, she had burns of forhead, eyelids, cheeks, left ear and neck. The right half of forehead burn was partial thickness. The burns of left half of forehead ranged from left upper eyelid to part
of the head. It was extensive and quite deep impression.
We debrided the blisters and loose skin. The burn from forehead to neck was sealed with Plusmoist(TM). The lesions of bilateral eyelids and cheek was covered with Duoactive(TM).
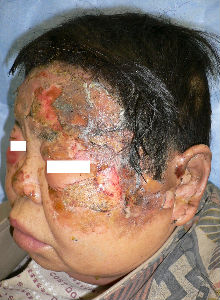
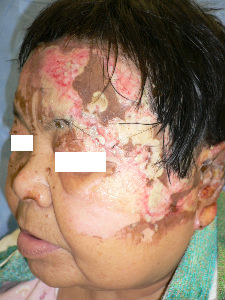
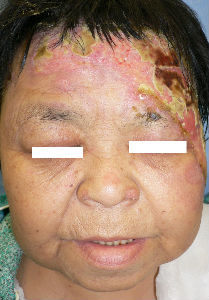
Day 6, the burn of her right cheek was re-epithelialized. Left cheek burn came to full-thickness necrosis. The necrotic tissue of forehead was quite thick. We evaluated that it was third degree burn. Left upper eyelid lesion was re-epithelialized within one week.
Day 17, She was discharged. As the outpatient, she came to our wound center twice a week. We educated her various methods, that she did at home. They included several dressings (eg. Plusmoist(TM)), direct sealing with wrap and others. She tried every methods and choiced the most comfortable one for herself. Necrotic tissue was liquefied by autolysis. We excised floating parts of necrotic tissue.
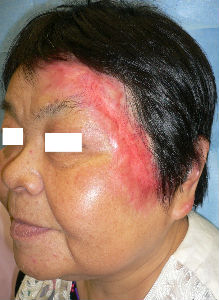
Day 59, most of forehead lesions ranging from left eyeblow to hairline were re-epithelialized. She covered the surface of granulation with food package wrap. Wearing scarf over it, she lived at home without problems. As the exudate form burn was not much, she never mind it and did not care about it.
Day 72, the ulcer on the front side of the left auricle was re-epithelialized. the large ulcer spreading from left eyeblow to the lateral canthus was seen.
Day 113, all lesions were completely re-epithelialized. Very mild scar contractures were seen.
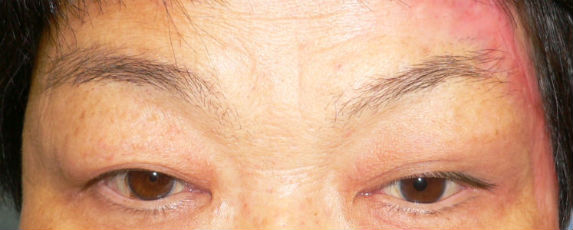
Day 164, we had last follow-up on her. She had no visible scar and pigmentation on her forehead. Compared with her right eyeblow, her left one was lifted a little. Opening and closing eyes were normally performed. She did not have complaints that difficulty in closing eyes and feeling dry eye.
 |
 |
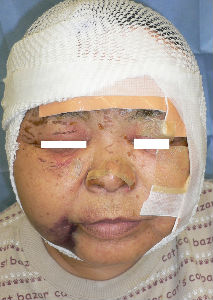 |
| the first day | oblique view | covered with Plusmoist(TM) and Duoactive(TM) |
 |
 |
 |
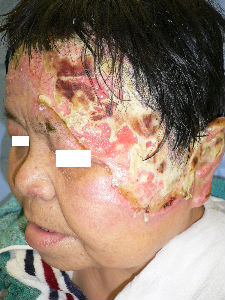 |
| 1 day after | oblique view | 3 day after | oblique view |
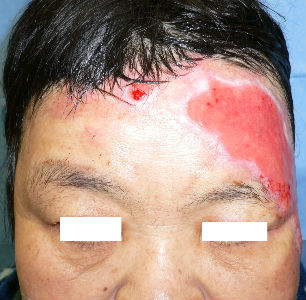 |
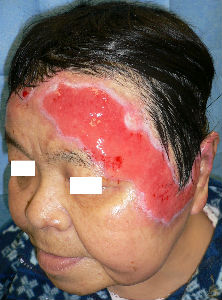 |
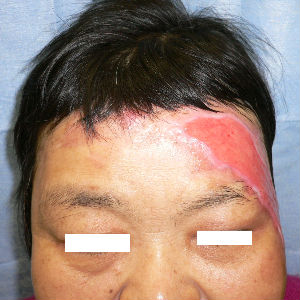 |
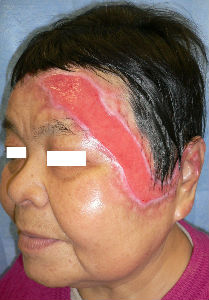 |
| 14 day after | oblique view | 45 day after | oblique view |
 |
 |
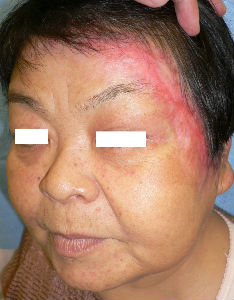 |
| 59 day after | oblique view | 113 day after |
 |
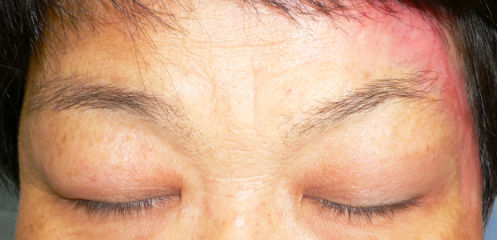 |
| 164 day after: open eye-lid | 164 day after: close eye-lid, no cicatrical contracture at left upper eye-lid |
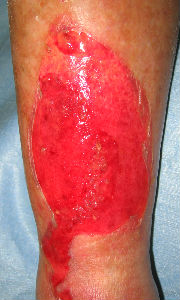
A 96-year-old woman was taken to our division for unknown cause burn in her front right lower leg. At the initial evaluation, the burn was partially covered with broken blisters and necrotic tissues
We removed the blisters, loose skin and necrotic tissues first. We evaluated that the burn was second degree burn (superficial dermal burn; SDB or deep dermal burn; DDB). There was white loose damaged tissue at right edge of the burn, which could be removed with tweezers. It was not surviving normal skin. When we tried to peel off it, she comlained pain. We left it as it was.
We sealed the burn with food packaging wrap that was coated with plenty of petoroleum jelly. We did not use disinfectants and antibiotics. We did not wash out the lesion.
We supposed that bandage should peel the fix site of normal skin when we exchange the dressing. We did not use bandage and wrapped around her lower leg.
Her family hoped that we treated her as outpatient. We educated her family the principles and the plan of treatment. We asked them to exchange the plastic wrap everyday and to take her to our division twice a week. They were fully educated and understood the theory of treatment very well.
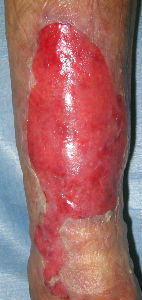
Day 7, most of the lesion was recovered with thin re-epithelialization tissue.
Day 12, the burn wound was completely re-epithelialized.
 |
 |
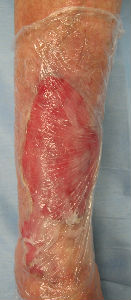 |
| remove the blister | covered with the food packaging wrap |
 |
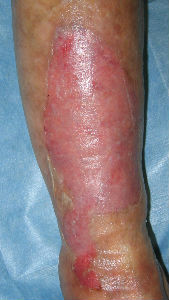 |
| 7 days after | 12 days after |
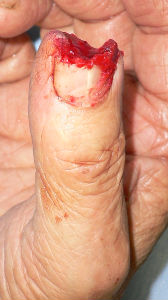
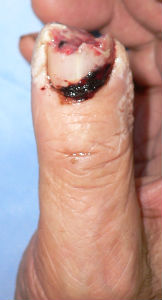
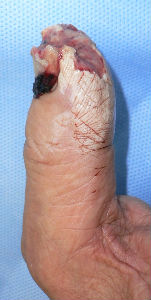
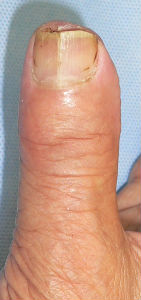
A man in his mid-70s chipped the tip of his right thumb with an electric saw, when he was cutting lumber. Immediately he visited to our hospital.
I covered this wound with alginate dressing. The tip of the distal phalanx was nibbled. The wound involved skin, soft tissue and bone at the distal 1/3 of nail plate.
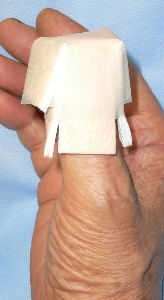
Next day, I covered the wound with Plusmoist(TM).
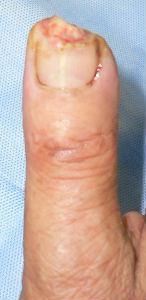
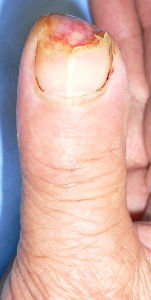
50 days after, the finger tip and the nail plate was completely regenerated.
 |
 |
 |
 |
| Primary condition | 1 day after | 1 day after lateral view |
covered with Plusmoist(TM) |
 |
 |
 |
 |
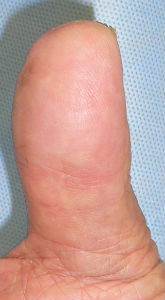 |
| 7 days after | 14 days after | 29 days after | 50 days after | 50 days after volar view |
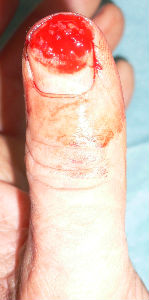
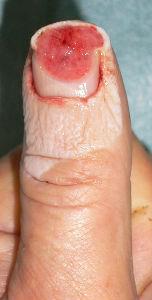
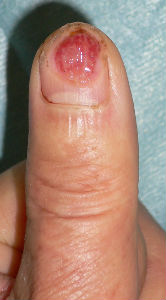
The patient is a 60 years old male worker; suffering from the cut wound of dorsal side of the left thumb visited our hospita. The wound was diagnosed as the defect of the nail plate and nail bed, complicated with the open bone fracture of the distal phalanx.
I attached the sodium alginate dressing. At the initial diagnosis, I removed the blood coagulation, attached the sodium alginate dressing on the wound and enclosed the wound by the film.
The day after the first visit, his nail bed was embedded by the surrounding healing granulation. I altered the dressing from sodium alginate dressing to Plusmoist(TM).
 |
 |
 |
 |
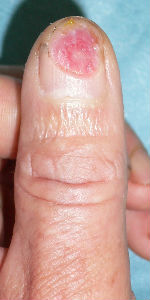 |
| the first condition | covered with alginate dressing | one day after | 11 days after | 21 days after |
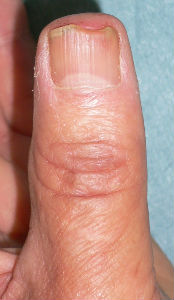
He chanced to re-visit our hospital on 94 days after, and I confirmed the complete reconstitution of the left thumb nail. The nail plate of his left thumb fully covered the nail bed, and fully recovered the intact nail form.
 |
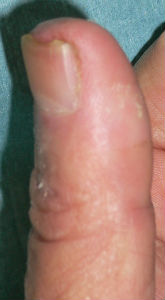 |
| 94 days after | lateral view |
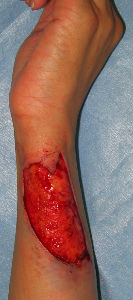
A female patient in her thirties visited our department immediately after her left forearm got caught in a machine at work.
Full-thickness skin loss, 9 cm in length and 6 cm in width, was observed on the ulnar surface of the distal left forearm. Wound irrigation was not performed, but alginate dressing was applied and the lesion was covered with a film dressing. No antibiotics were administered. Alginate dressing was immediately applied.
Next day, irrigation and application of Plusmoist(TM). The patient had almost no pain when the lesion was washed.
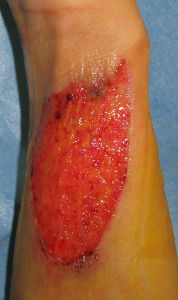
Six days later, the wound surface was covered by clean granulation tissue, but the size of the wound remained unchanged. There was nothing particularly noted during the clinical course. She had no pain during exercise and was able to perform her daily housework.
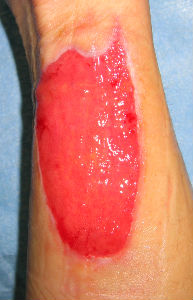
Although 49 days had passed, the wound had not reduced in size to a great extent; only the wound on the distal back side was slightly smaller. However, she had no pain during exercise and was able to perform her daily chores.
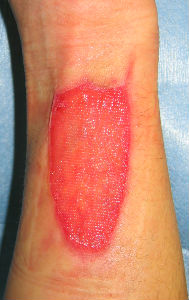
About 2 months after the incident, the width of the wound had shrunk, but the length of the wound had not changed to a great extent. The width of the wound was little larger than 1 cm at 83 days after the incident.
Only a shallow ulcer remained in the center of the wound at 97 days after the incident, and the entire wound had epithelized at 104 days after the incident. Follow-up was performed until 139 days after the incident. Only a mild scar remained. No contracted scar was observed, and she experienced no differences in the movements of the forearms as well as the wrists. In addition, she had no feeling of stiffness.
Now, you might have a different view with regard to the treatment of this case, for example:
 |
 |
 |
 |
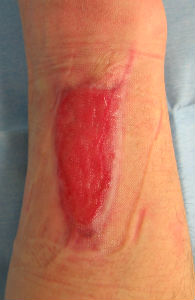 |
| primary condition | 6 days later | 21 days later | 49 days later | 76 days later |
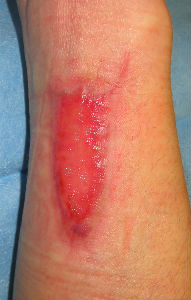 |
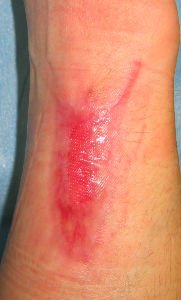 |
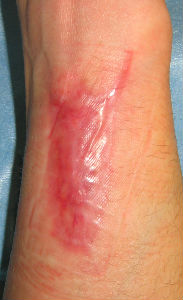 |
 |
| 83 days laterr | 97 days laterr | 104 days laterr | 139 days laterr no cicatrical contracture |
The following aspects of the issue have to be excluded: the physician's convenience and thephysician's imposition of good will. Physicians tend to consider that "rapid treatment and accelerating wound healing are good." However, they are not necessarily "good" for patients.
For instance, it would not be the best outcome for the patient if his/her body movement is limited and a dysmorphic disorder remains as a result of accelerated wound healing. Although the time the physician spends with the patient is limited, the patient has to use his/her body for the rest of his/her life. In other words, the time required by the physician for determining the result of the treatment is completely different from that for patients.
Surgery is necessary to treat wounds rapidly, but if some impairment remains for the rest of the patients' lives (even if it is a mild impairment), such a treatment is considered a failure. Grafted skin definitely causes a contracted scar. If it is inevitable, skin grafting is the worst treatment for patients.
Thus, it is wrong to perform a therapeutic evaluation on the basis of thephysician's logic. For example, even if a chef cooks using a great technique, he fails if the dish tastes bad. Thus, there is a bias if the person who cooks the dish is not different from the person who assesses it.
However, in the medical sciences, physicians perform both therapeutic evaluation and surgery. The problem lies in the fact that no one is concerned about this abnormality.
First, the following data was revealed in this case:
In other words, it took several months for complete epithelization, but the scar was undistinguishable and no movement disorder developed; this allowed the patient to perform normal daily activities and work during the treatment period. In fact, I have the impression that the body adjusts to the duration of epithelization in order to suppress wound contraction, which causes movement disorder.
The same phenomenon as that in the case of "wide range of third-degree burn wounds on the forehead," which I had reported in the past, can be considered here. It took several months for complete epithelization; however, as a result, the patient showed no limitation of eyelid movement or sequelae.
With respect to these cases, the time lags from covering of the wound surface with granulation tissue to the onset of wound contraction is considered to be the required duration for the granulation tissue to obtain the mobility required for the region. Moreover, it is considered that the body is “waiting” for the best time to achieve the required mobility in regions that take time to epithelize.
Thus, I believe that epithelization does not take a long time, but the body "waits" for a condition in which it requires the shortest time to regenerate granulation tissue and dermis, according to the amount of physical activity in this region.
Given this perspective, it is possible to explain why contracture occurs after skin grafting: When skin grafting is performed at an early stage, the granulation tissue of the graft bed is immature and has not yet had the required amount of physical activity in this region. It is considered that movement disorders are caused by a skin graft that covers all the granulation tissue in such conditions.
Therefore, for wound epithelization without movement disorders, it is first necessary to generate granulation tissue (= the base of the regenerating epithelium) that responds to the requirement that no movement disorder develops. Second, it is necessary to regenerate flexible skin on the base. It is considered that it takes a long time to achieve it. Skin grafts “steal” the time required for it.
Why is skin grafting the worst treatment? Because skin grafts tentatively cover the wound without "waiting" for regeneration of the tissue (= granulation tissue) required to allow physical activities; this causes skin contracture and results in movement disorders of the contracted scar. When a skin graft is performed, "the wound will heal quickly but contracture will develop later." However, this is a natural phenomenon.
In addition, healthy skin has to be collected for skin grafting; this means that healthy parts of the skin have to be peeled and grafted.
At this point, majority of the plastic surgeons consider that “there is no problem because the skin is collected from a region that cannot be seen,” but this is wrong as they only think about their convenience. They do not consider the patient who will have scars in an uninjured region.
Patients would have a scar in a region that did not get burned, but the physicians would not have any scars. Physicians do not feel any pain when they cause "new scars." Thus, they persuade patients, stating that "there is no problem in collecting the skin because the region cannot be seen." They do not know how much pain the patient experiences in order for them to be able to perform a skin graft.
Curing a wound at an early stage and having the patient discharged promptly is not necessarily "good" for the patients. As far as skin grafting is concerned, I have no doubt that curing a wound at an early stage by using skin grafting results in the worst result.
I am expecting objections and counterarguments from plastic surgeons and dermatologists who prefer to perform skin grafting.
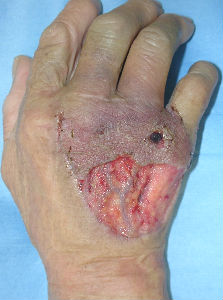
A about 70-year-old woman presented with dog bite avulsion to the back of her right hand. She had large skin soft tissue defect in her right hand. Some extensor tendons were exposed in the wound.
We washed out the wound under local anesthesia. The laceration part of the wound was sutured as possible. We applied alginate dressings on it. The injury day, we gave tetanus toxoid and antibiotic Cefazolin. Day 3, we confirmed that no infection signs was seen in her wound. We do not administered antibiotics during the subsequent course of treatment. In the early period, we used TielleTM as dressings. In the latter period, we changed dressings to ALLEVYNTM.
We educated her to use her hand actively for prevention of contractures.
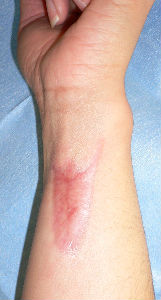
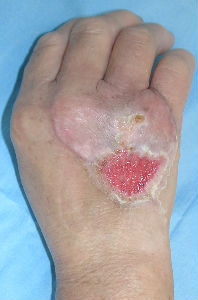
Day 42, the wound was re-epithelialized completely. Neither muscle contractures nor scar ones were seen in her right wrist joint and MP joints. No differences in range of motions were seen between her bilateral hands.
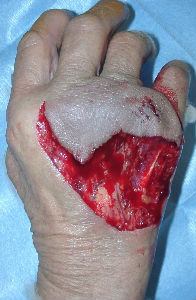 |
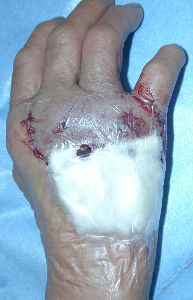 |
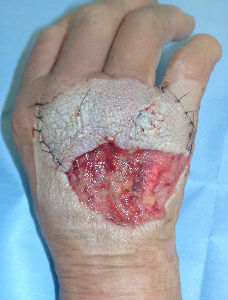 |
| the first condition | covered with alginate dorreessing | 3 days later |
 |
 |
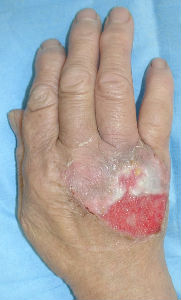 |
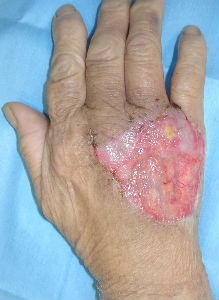
| 6 days later | 11 days later | 17 days later |
 |
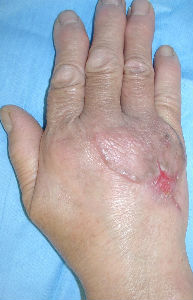 |
| 24 days later | 42 days later |
#1. Miliaria (an itchy rash of small raised red spots) or impetigo(a superficial skin infection)
Skin is one of the excretory organs. Sealing the skin causes dysfunction of excretion. It can cause miliaria or impetigo. For preventing these skin problems, dressings have to be changed everyday after washing the wound with plenty of tap water.
#2. Wound infection
Detection of infection is important. Infection does not mean that bacteria are found in the wound. Signs of infection include pain and/or redness at the site. If the wound becomes infected, the infected site must be removed. Antibiotics are not needed for the patient whose symptoms disappear following these measures.
#3. Granuloma(thickening of skin at the wound site) formation
Sealing the wound with steroid ointment covered dressing, the granuloma becomes flat and the wound resumes epithelialization(healing of the wound) .
Makoto Natsui (MD), e-mail, JAPAN